Radiological diagnosis:
EPS is such a rare entity,
even in its secondary form,
that there is no consensus or protocols for emergency abdominal imaging.
We here present 3 cases of surgically proven idiopatic SEP and their radiological signs and we depict radiological findings and describe the different imaging techniques used for the diagnosis of SEP in the emergengy setting.
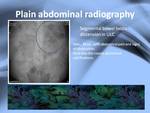
Abdominal radiography:
Plain abdminal radiography can show air-fluid levels or bowel dilation (Fig.
6),
even peritoneal or mesenteric calcifications but abdominal X-rays can appear normal.
Given the rarity of the entity no sensitivity or specificity data are available
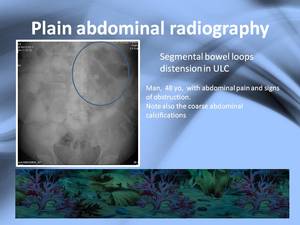
Fig. 6: Plain abdominal radiography: bowel loop distensión in the LUC
Ultrasonography (US):
US may detect abnomal bowell loops with tethering or bowell distension as well as encapsulated ascitis.
Echogenic strands and membranes are described in secondary SEP,
but no data is found regarding idiopathic SEP.
Computed tomography:
Already used for secondary SEP as long as in 1988,
CT is the main tool for the preoperative diagnosis of SEP.
On an emergency seting obstruction signs will be found,
with dilated bowel loops and air-liquid levels.
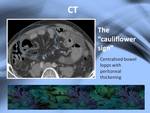
The small intestine will usually be found accumulated and aglomerated in the center of the abdomen,
apperance described as "the cauliflower sign",
clue to the diagnosis of SEP.
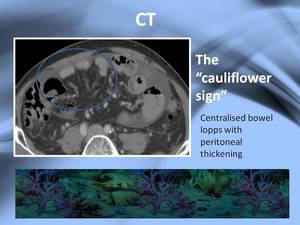
Fig. 7: The cauliflower sign
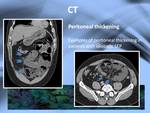
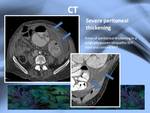
Although the cauliflower sign is the most characteristic sign of this entity peritoneal thickening is also characteristic (Fig.
8).
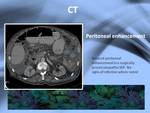
The peritoneal thickening can show hiperenhancement,
what will raise the differential with inflamatory or infectious peritoneal disseases (Fig.
9).
Although some authors have described peritoneal calcification in our series none of the patients with idiopathic SEP presented that finding,
although peritoneal engorgement could be quite impesive as in figure 10.
Only in one case mesenteric calcification was seen.
(Fig 11)
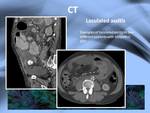
The peritoneal fibrosis causes loculation of ascitic fluid,
being this another ancilary finding that helps the diagnosis of SEP (Fig,
12).
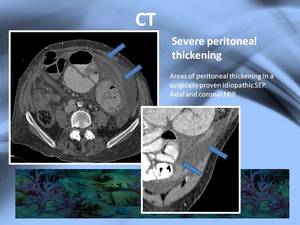
Fig. 10: Massive peritoneal thickening
Although most articles require surgery and histology for a definitive diagnosis Vlijm et al (ref.
3) describe a 100% sensitivity and a 94% specificity for the diagnosis of secondary SEP in patients with peritoneal dialisis.
Other imaging techniques:
Baritated studies,
MRI or even fluordeoxyglucose PET have been also reported in the diagnosis of SEP,
although those techniques are not ussually available on an emergency setting.
Diferential diagnosis:
Idiopathic SEP is one uf the most unusual conditions that lead to intestinal obstruction.
The differential must be established with conditions that appear with anomalous possition of small bowel,
peritoneal thickening or loculated ascites.
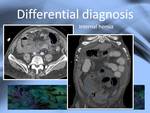
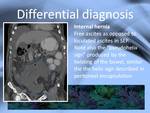
Peritoneal encapsulation and internal herniation are the two entities that should be primarily considered.
In internal hernias look for free fluid and absence of peritoneal thickening.
On both pathologies the position of the bowel can resemble "the helix sign" described in peritoneal encapsulation.
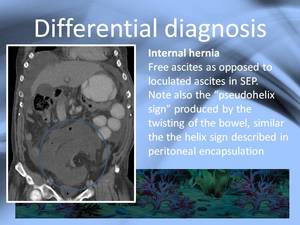
Fig. 14: Internal hernia resembling the "helix sign"
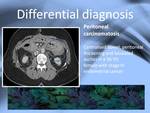
Disseminated oncologic dissease can also mimic ESP,
finding anomalous position of small bowel ,
loculated ascites and peritoneal thickening,
usually nodular,
but sometimes also smooth peritoneal thickening can be seen as in fig.
15.
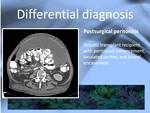
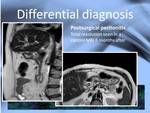
Infections must be included in the differential and specially peritoneal tuberculosis must be ruled out in areas with a high prevalence of the dissease.
Although it is the most characteristic differential for SEP other infections causing peritonitis can resemble the dissease as shown in fig.
16.
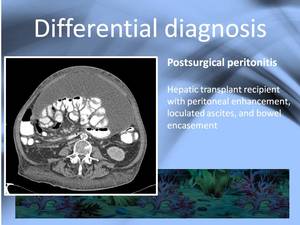
Fig. 16: Post transplant peritonitis